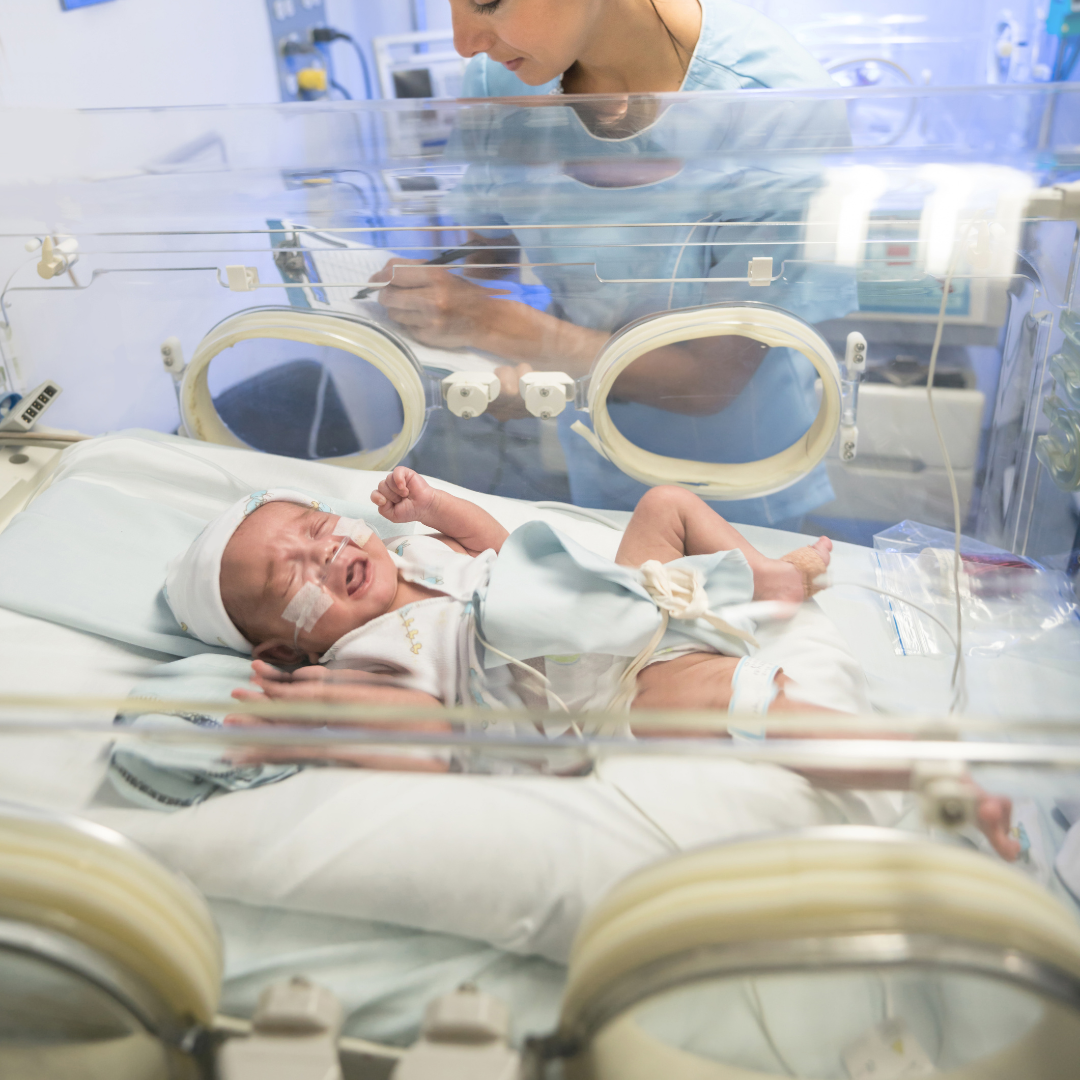
One of the most difficult aspects of parenting in the NICU is sharing big decisions and large amounts of time with a lot of other people.
And sometimes it’s A LOT of people!
Doctors, residents, surgeons, nurses, therapists, volunteers, respiratory therapists, other parents…whew. Lots of personalities and lots of opinions. And sometimes… personalities clash.
If you’ve ever had a hard time navigating a relationship with your baby’s bedside nurse, provider or other medical staff member… we’re going to talk through some things that may be helpful to think about.

I want to start off with a little story. Something that gives you a peek into an aspect of the NICU world we experience sometimes as providers, but isn’t really talked about.
Here we go.
So, I was hanging around in the NICU unit one day. I was chatting with a group of incredible nurses at the nursing station about a patient and their family when a nurse said, “Yeah, I got fired.”
Hmm…now, you may be assuming that means the nurse caring for the child was fired from her position at the hospital, but in reality, she was talking about how the nurse had been fired by the NICU family.
“But Katie, what does that mean?”
Essentially, the NICU family didn’t want that specific nurse to care for their child. So they asked that she not be on their child’s care team anymore.
Y’all, it feels harsh as I type it, and it kind of is.
BUT, navigating relationships in the NICU, navigating trauma and tension and stress…it’s not easy (if you’ve been in the NICU, then you know). We don’t “get along” with everyone, and tension can run high in such a high-stakes environment.
That’s why we’re going to walk through some strategies to increase your peace & build your confidence in navigating difficult provider-family relationships.
I HAVE to add…the nurse that was “fired” is dang AMAZING. She cares deeply for her patients, she goes the extra mile for families, and she has a kind and approachable personality. We get along incredibly well, and I would choose her to care for my child if they were in the NICU.
Soooo, if that’s true, what happened??
I won’t dive into the specifics of this specific situation, but there’s a lot of factors that may contribute to tense relationships between NICU providers and NICU families.
- Varying strengths and weaknesses
- Different personalities
- Different priorities for the baby’s care
- The overall medical situation and concerns
- Different backgrounds and values
- Everyone has a different way of providing care
- That resting face (you know what I’m talking about…)
- Is family-centered care valued?
- What is going on behind the scenes in someone’s personal life?
- The overall NICU culture
And on and on.
Let’s look at a couple things that may help ease your mind and help you foster more successful relationships and greater peace of mind on your NICU journey.
Tip #1: Create a primary nurse list.
Have you heard of a primary nurse?
Primary nursing is when you get to choose a nurse you “like” and get along with, and who knows your baby to take care of your baby consistently when they are on the schedule.
So, if your primary nurse is working that day, they will be assigned to your baby.
Now, this may or may not be possible within your NICU, but it’s DEFINITELY something you can ask about. If it’s an option, I would highly recommend taking advantage of it.
It’s natural that we may click better with one person than another.
Benefits of primary nursing in the NICU:
- Consistent provider=consistent care!
- Greater familiarity with patient’s history and preferences
- Decreases parent anxiety
- Parents show an increased trust in the medical team
- Greater opportunity to develop a meaningful relationship between parent and provider
If you’re curious whether or not your unit practices primary nursing assignments, ask to speak with the charge nurse, or simply ask your baby’s bedside nurse today whether that’s an option.

Tip #2: Prioritize improving communication.
Did you know most conflicts that occur between a medical team and patient comes down to communication?
Sometimes, communication just doesn’t match up.
It’s tough to communicate well in the NICU sometimes. We can get fiery, passionate and opinionated (Can I get an amen?).
Give yourself some grace and try some of these tips to improve the communication between you and your baby’s care team.
- Be aware of nonverbals like facial expressions and tone of voice.
- Make your requests known (in a kind and compassionate way!)
- Avoid talking bad about one another behind closed doors (this really just pours gasoline on your feelings and frustrations)
- Validate their feelings and empathize FIRST, before jumping in to problem solve or frame your opinion.
For example, maybe you wanted to hold your baby, but when you arrive, their nurse has already finished their assessment and tucked them back into bed.
Since we like to avoid waking babies up, she may request you wait to hold your baby until the next care time.
Cue…frustration (and naturally so!).
But, here’s the thing. BOTH of you are doing what is right for your baby. Your nurse wants to protect their sleep, and you want to hold and spend some time bonding.
Next time, communicate ahead of time.
Let your nurse know you’re going to be there at their care time and you want to hold. This helps your nurse plan their day and coordinate any care that is needed.
Tip #3: Allow for flexibility with things that don’t matter as much to you.
Let’s do a little exercise.
Go ahead and think through and decide on 3 to 4 things that matter the most to you as a NICU parent. You can even write them down if you want so you can come back to them.
- Is it being there for the firsts? Like the first bath or first bottlefeed?
- Is it feeling like a member of the team and having a chance to ask your questions?
- Is it talking to your baby’s providers in person?
- Is it having someone who you just get along and vibe with?
- Is it getting to do your baby’s care?
- Is it knowing what to expect during your visit?
Now, I know all of it is important to you!
It can help to prioritize the things that you don’t want to compromise on and make sure those are known to your baby’s team.
If there’s something bothering you AND it’s related to your priority list, it may be time to speak up and either request a different provider, or let your baby’s nurse know your preferences.
On the road to a more peaceful mind, it can be impactful to focus more on what truly matters to you than stress over things that you can let go.
Tip #4: Ask yourself some questions before confronting someone or requesting a change.
This is kind of a “touchy-feely” post. I totally get it if the last thing you want to do is think before you speak (especially when the mama bear feelings come out!).
The goal here is to SLOW DOWN. Slow down those intense moments that sometimes erupt in the NICU space.
Peek at some of these questions you can ask yourself before you confront someone in the NICU you’re not getting along with, or before you request a change in your care team.
- “Does this really matter to me? Is it on my priority list?
- “Will this matter to me tomorrow?”
- “Is this an isolated concern or have I been having repeated concerns?”
- “Do I have issues or concerns related to safety and trusting this person with my baby, or do we just have clashing personalities?

Tip #5: Speak with the charge nurse.
When it comes down to it, you need to trust your care team.
But it’s also important to remember that NICU providers should be respected for their efforts and service as well (and 98% of the time, they are!).
If you are navigating a difficult situation and not sure how to proceed, or have safety concerns…it may be time to address it with the unit charge nurse.
The charge nurse or nurse manager is responsible for overseeing the nurses in their clinical roles. Their job is to mediate and manage all-the-things. As always around here, I want to remind you to approach every conversation with compassion and humility.
At the end of the day, we are all people navigating life, and we’re all on the same team. Your baby should be at the center of care.
It’s true that sometimes NICU providers and family just don’t seem to get along. BUT, it’s important to acknowledge that more often, NICU families develop magical, trusting, and deeply rooted relationships with their care team.
There’s a trust and bond that can develop in the NICU that very few in the world understand.
You’ve got this.
Let’s make the NICU a better place, together!