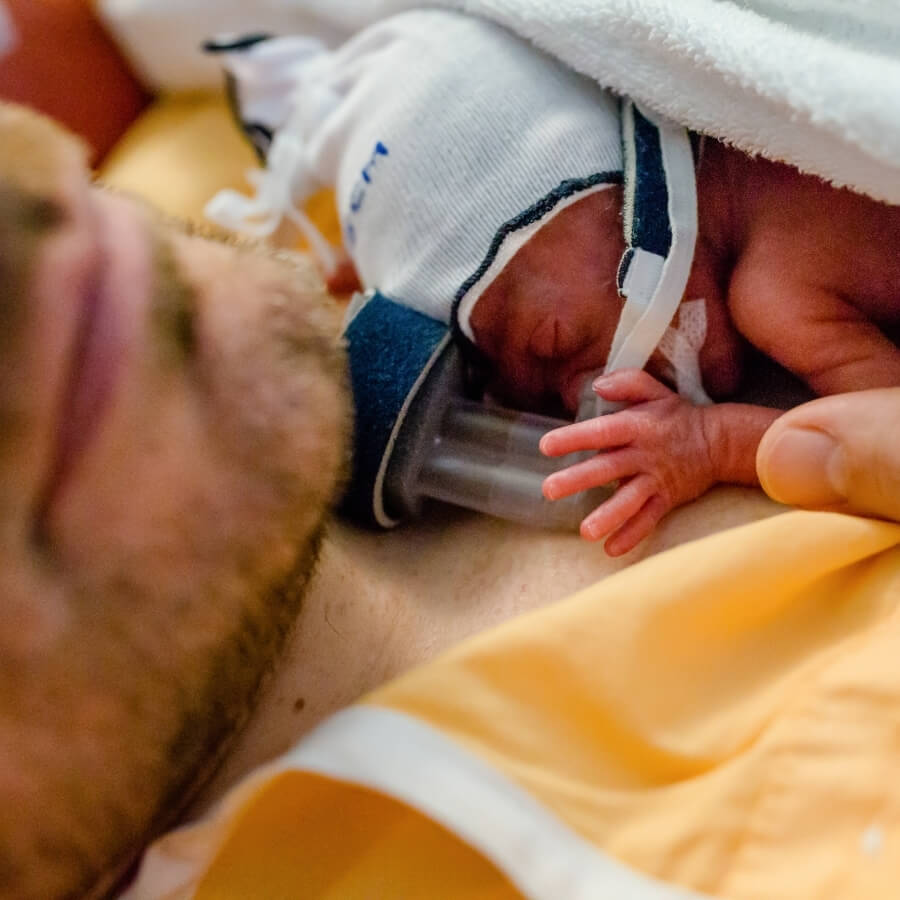
There are a lot of factors that affect a NICU baby’s tolerance and enjoyment of skin-to-skin holding. If your baby’s monitor alarms, they seem uncomfortable, or if they have a difficult time settling in, read on! Spoiler! It’s not you! I’m sharing 7 ideas for you to discuss and explore with your baby’s nurse with the goal of creating a successful, positive, and relaxing kangaroo care session!

I had a mom tell me once that she didn’t want to hold her baby skin-to-skin, because she caused her baby to have more “desats” (oxygen dips). Wow, my heart, y’all.
I want you to know there is a lot more to the puzzle!
Your baby is complex.
If you have ever felt like you are the reason why your baby is dropping her oxygen or heart rate during kangaroo care, I hope learning about the complexities of your baby will relieve you of that guilt and fear.
Please know this is not an exhaustive list (by any means!), and I am not at your baby’s bedside to provide an individualized recommendation or assessment of your baby. I simply want to share the many things that may impact a baby’s tolerance during a kangaroo care session.
I want you to hear this. It is not because of you!
Let’s jump into a couple of things you can think about, discuss with your bedside nurse, and try, when supporting your baby during skin-to-skin care.
1. MAKE SURE YOU HAVE MAXIMAL SKIN-TO-SKIN CONTACT
You know what that means?
That’s right mama, I want you to remove your bra for skin-to-skin.
It’s a common choice to leave your bra on during skin-to-skin, BUT, if you’re comfortable, and have certain supports in place (like privacy screens, a private room, a cardigan to wear, or if your hospital provides a hospital gown to cover up)—I would love for you to remove it.
I have a couple of reasons why.
-
Allows for direct contact with your skin
Without your bra, your baby’s legs, belly, chest, feet, hands and arms are all in direct contact with your skin. This provides your baby with the MAX benefits of a skin-to-skin care experience. If we’re going to get that baby out, let’s set them up for success by providing them with the most supportive holding place possible…mama’s SKIN!

-
Provides better temperature stability.
Did you know that when your baby is skin-to-skin, your body warms up and cools down in response to their temperature?
You are regulating your baby’s body while they are out of their isolette. If there is a barrier, like a piece of clothing (i.e. the bra!) between your skin and your baby’s skin, your baby’s temperature isn’t being regulated by your powerful skin!
You have the best influence on supporting your baby’s temperature stability by making sure the receptors on your skin are in contact with theirs.
2. DO A STANDING TRANSFER FOR KANGAROO CARE
How is your baby moving from their crib/isolette/warmer to your arms?
Does it feel like they’re being flopped on your chest?
Is your baby seemingly flying through the air?
If they are, then the stress of the transfer may be making it harder for them to re-organize once they’re on your chest (aka: their happy place!).
There are several transfer methods for getting your baby out to hold skin-to-skin. If you are physically able (and your baby’s nurse is trained!), a standing transfer is the safest and most supportive method!
You may already know how to do one, or be doing it with your nurse without even realizing it.
-
HOW DOES A STANDING TRANSFER WORK?
A standing transfer means whoever is holding the baby, mom or dad, is standing at the bedside and bends over to bring their chest down to their baby then stands up with the baby on their chest.
No flying through the air.
Your baby goes straight from their bed/isolette/warmer to mama’s skin. The bedside nurse is responsible for managing lines and tubes, and ensuring further safety of the transfer.
3. DECREASE ENVIRONMENTAL INPUT
What does the environment surrounding your baby’s bed space look like?
Are you in an open-bay style NICU where beds are right next to one another?
Do you have a private room?
What about ALL the things your NICU baby is hearing, smelling, touching, seeing, feeling?

When your baby comes out of the isolette for skin-to-skin, they’re no longer protected by their incubator.
This can play a major role in your baby’s tolerance to skin-to-skin care.
Think about things that may be stressful or overwhelming for your baby to process while they’re out being held.
- Are the lights really bright?
- Are your baby’s eyes shielded?
- Is it a noisy bed space?
- Are nurses talking at the nursing station?
- Is there a baby being admitted next to you?
- Are there alarms or ventilators beeping?
Without mature self-regulation, your baby may respond with a bradycardic event (decrease in heart rate) or desaturation event (decrease in oxygen). Your baby is learning to process different types of input at one time (a really hard task!).
Prioritizing skin-to-skin can help build your baby’s coping skills and assist with sensory integration and sensory processing skills.
When preparing for skin-to-skin care (BEFORE getting your baby out!), take a look at the environment around you and ask these questions:
- Is this environment relaxing for my baby?
- What can I do to create a more comforting environment for my baby?
Start a discussion with your bedside nurse or neonatal therapist, so you can troubleshoot and create the most POSITIVE experience possible for your baby AND you!
4. PREVENT COLD STRESS
Cold stress is your baby’s response to inadequate temperature regulation.
If your baby is a preemie, they aren’t able to maintain their own temperature. That’s why they are placed in an isolette or on a warmer bed. As they get older, their sweet body will learn to manage their own temperature.
Term babies in the NICU can also be susceptible to cold stress and need support.
Think about getting out of a hot tub on a cold day…brrrrr. Your body tenses up, and it almost takes your breath away.
BUT, if you were wrapped in a warm towel before getting out, you would feel MUCH WARMER, and your body would have a lower stress response.

Transitioning to skin-to-skin care has the potential of exposing your baby to the air, resulting in cold stress (depending on their age and medical stability).
When a baby experiences cold stress, they may have a medical response like a drop in their heart rate or oxygen rate. OR, they could show you a variety of other stress signs, like the hiccups or stiffening their legs.
Talk with your nurse or neonatal therapist about ensuring your baby’s skin is minimally (if ever!) exposed to the outside air without a source of warmth.
- Use the warm blanket/pad/positioning device under them to cover their back during the transfer.
- Swaddle them first.
- Complete a standing transfer, so your baby is on your chest as quickly as possible.
- Put a hat on your baby before getting them out.
The good news is…we can minimize cold stress by changing how we do a transfer.
5. AVOID STUFFING BABY DOWN YOUR SHIRT
Yep, been there, done that.
You’re wearing a v-neck shirt to visit your baby, you hold it open, and the nurse places your baby down your shirt and onto your skin.
Instead of getting those arms and legs stuck on the opening of your shirt, ask for a hospital gown, remove your shirt, and put the hospital gown on like a robe (remember, no bra either ?). That way your baby goes straight to your chest.
It’s difficult to do a standing transfer with the “stuff down the shirt” method.
Removing your shirt makes the transfer easier, and decreases the likelihood your baby will become stressed, overwhelmed, caught, or stuck.
6. ALLOW BABY TO WIGGLE WHERE THEY WANT (WITHIN REASON!)
Did you know there was a research study that came out looking at a specific position to place baby during skin-to-skin?
Guess what it found?!
Babies HAD TONS of positive responses to being placed in a supported, diagonal flexed position on their mama’s chest (Source).
I’m not surprised based on my experience with babies and skin-to-skin holding–those babes are wiggly!
Babies often wiggle their way to a DIAGONAL position on mom‘s chest during kangaroo care.
This is actually a beautiful developmental response.

Babies are born with the innate desire to transition to the breast, even preemies! Your baby likely smells your milk and wants to be near that liquid gold.
Instead of constantly re-positioning them, if your baby is comfortable lying diagonally on your chest…let them rest there. Just check to be sure they are…
- supported in flexion,
- showing signs of comfort,
- medically stable, and
- their lines and tubes are secure.
7. RECOGNIZE BODY SYSTEM RESPONSES
Your baby is feeling ALL OF THE FEELS.
Just like we can feel hungry, tired, sore, get a stomach ache, headache, gas pains, reflux, etc…so can our babies.
If your baby is having a difficult time tolerating kangaroo care, they may be trying their best to deal with the many different ways their body feels.
Does your baby battle reflux?
Is their NG/OG feed going in?
Does your babe have GI distress?
Your baby is learning to process the way their body feels. Sometimes their response to discomfort or pain will be to drop their oxygen or heart rate.
They’re building self-regulation skills, but they need our help to get there. As your baby gets more mature, they will grow more successful at coping with all kinds of input.
If you want to help your baby build good coping skills and learn to regulate their environment, check out this post, 5 WAYS TO HELP YOUR BABY LEARN COPING SKILLS IN THE NICU.
I hope learning about some of these things helps you brainstorm with your nurse or neonatal therapist about how best to support your baby.
Let me repeat, if your baby has episodes during kangaroo care, it’s not because of you!
Prioritize skin-to skin holding with your baby.
It’s one of the absolute BEST things you can do for them!
Medicine only parents can provide!
You’ve got this,